Overview
Junctional epidermolysis bullosa
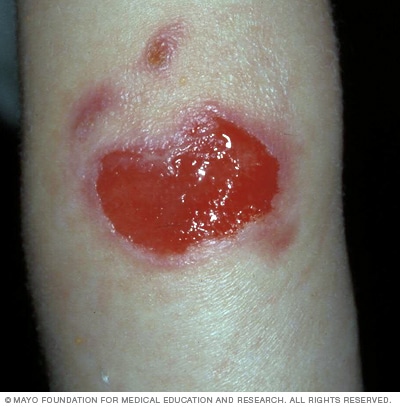
Junctional epidermolysis bullosa
Junctional epidermolysis bullosa can show up at birth. Large, open sores are common and can lead to infections and loss of body fluids. As a result, severe forms of the disease may be fatal.
Epidermolysis bullosa (ep-ih-dur-MOL-uh-sis buhl-LOE-sah) is a rare condition that causes fragile, blistering skin. The blisters may appear in response to minor injury, even from heat, rubbing or scratching. In severe cases, the blisters may occur inside the body, such as the lining of the mouth or stomach.
Epidermolysis bullosa is inherited, and it usually shows up in infants or young children. Some people don't develop symptoms until they're teens or young adults.
Epidermolysis bullosa has no cure, but mild forms may improve with age. Treatment focuses on caring for blisters and preventing new ones.
Products & Services
Symptoms
Epidermolysis bullosa symptoms include:
- Fragile skin that blisters easily, especially on the palms and feet
- Nails that are thick or unformed
- Blisters inside the mouth and throat
- Scalp blistering and hair loss (scarring alopecia)
- Skin that looks thin
- Tiny pimple-like bumps (milia)
- Dental problems, such as tooth decay
- Difficulty swallowing
- Itchy, painful skin
Usually epidermolysis bullosa blisters are noticed during infancy. But it's not uncommon for them to appear when a toddler first begins to walk or when an older child begins new activities that cause more friction on the soles of the feet.
When to see a doctor
Contact your health care provider if you or your child develops blisters for an unknown reason. For infants, severe blistering can be life-threatening.
Seek immediate medical care if you or your child:
- Has problems swallowing
- Has problems breathing
- Shows signs of infection, such as warm, painful or swollen skin, pus, or an odor from a sore, and fever or chills
Causes
Basement membrane zone
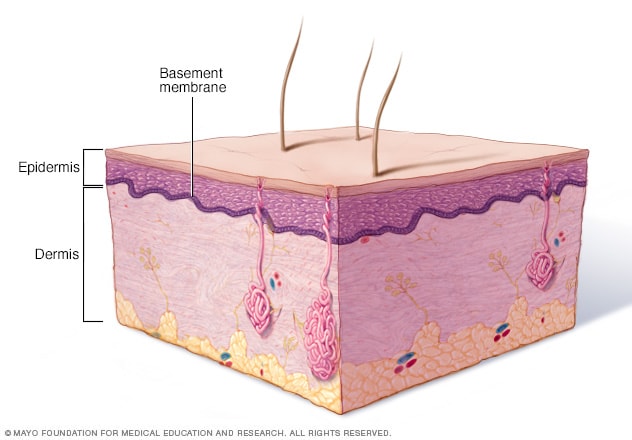
Basement membrane zone
Depending on the type of epidermolysis bullosa, blistering may occur in the top layer of skin (epidermis), the bottom layer (dermis) or the layer that separates the two (basement membrane zone).
Autosomal dominant inheritance pattern
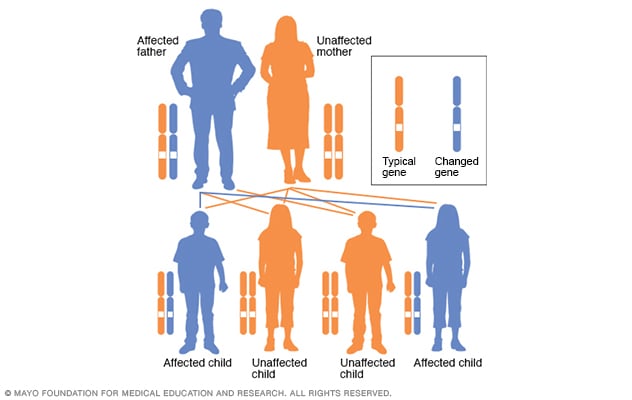
Autosomal dominant inheritance pattern
In an autosomal dominant disorder, the changed gene is a dominant gene. It's located on one of the nonsex chromosomes, called autosomes. Only one changed gene is needed to be affected by this type of condition. A person with an autosomal dominant condition — in this example, the father — has a 50% chance of having an affected child with one changed gene. The person has a 50% chance of having an unaffected child.
Autosomal recessive inheritance pattern
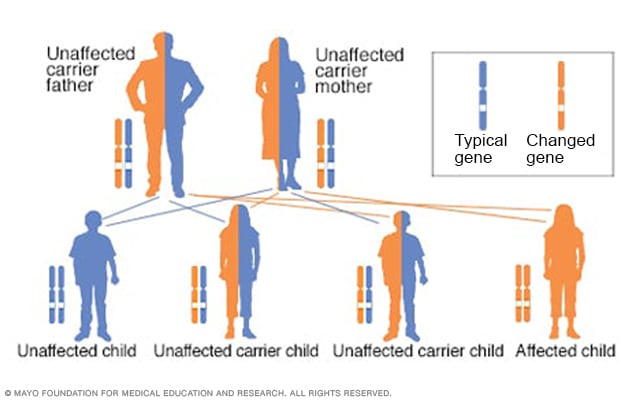
Autosomal recessive inheritance pattern
To have an autosomal recessive disorder, you inherit two changed genes, sometimes called mutations. You get one from each parent. Their health is rarely affected because they have only one changed gene. Two carriers have a 25% chance of having an unaffected child with two unaffected genes. They have a 50% chance of having an unaffected child who also is a carrier. They have a 25% chance of having an affected child with two changed genes.
Epidermolysis bullosa simplex
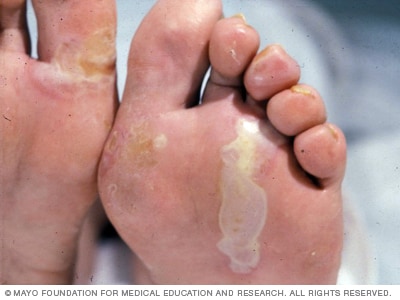
Epidermolysis bullosa simplex
Epidermolysis bullosa simplex usually becomes apparent at birth or during early infancy. It's the most common and least severe type. Blistering may be mild when compared with other types.
Dystrophic epidermolysis bullosa
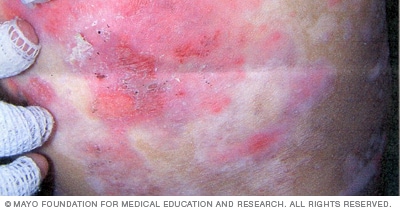
Dystrophic epidermolysis bullosa
Dystrophic epidermolysis bullosa generally becomes apparent at birth or during early childhood. The more-severe forms can lead to rough, thickened skin, scarring, and misshapen hands and feet.
Epidermolysis bullosa is caused by an inherited gene. You may inherit the disease gene from one parent who has the disease (autosomal dominant inheritance) or from both parents (autosomal recessive inheritance).
The skin is made up of an outer layer (epidermis) and an underlying layer (dermis). The area where the layers meet is called the basement membrane. The types of epidermolysis bullosa are mainly defined by which layers separate and form blisters. The skin injury might be brought on by a minor injury, bump or nothing at all.
The main types of epidermolysis bullosa are:
- Epidermolysis bullosa simplex. This is the most common type. It's brought on by heat and friction and develops in the outer layer of skin. It mainly affects the palms and feet. The blisters heal without scarring.
- Junctional epidermolysis bullosa. This type may be severe, with blisters beginning in infancy. A baby with this condition may develop a hoarse-sounding cry from continual blistering and scarring of the vocal cords.
- Dystrophic epidermolysis bullosa. This type is related to a flaw in the gene that helps produce a protein that glues the skin layers together. If this protein is missing or doesn't function, the layers of the skin won't join properly. It can cause skin that looks thin. Diseased mucous membranes can cause constipation and make it hard to eat.
- Kindler syndrome. This type tends to cause blisters in multiple layers and so can look very different from person to person. The blisters tend to show up in infancy or early childhood. It increases sun sensitivity and causes skin to look thin, mottled and wrinkly.
Epidermolysis bullosa acquisita is distinct from these conditions, as it isn't inherited and it's rare in children.
Risk factors
The major risk factor for developing epidermolysis bullosa is having a family history of the disorder.
Complications
Epidermolysis bullosa can worsen even with treatment, so it's important to spot signs of complications early. Complications may include:
- Infection. Blistering skin can become infected by bacteria.
- Bloodstream infection. Sepsis occurs when bacteria from an infection enter the bloodstream and spread throughout the body. Sepsis can spread rapidly and lead to shock and organ failure.
- Fusion of fingers and changes in the joints. Severe forms of epidermolysis bullosa can bind together fingers or toes and cause unusual bending of the joints (contractures). This can affect the function of the fingers, knees and elbows.
- Problems with nutrition. Blisters in the mouth can make eating difficult and lead to malnutrition and anemia, such as low iron levels in the blood. Problems with nutrition can also cause delayed wound healing and slowed growth in children.
- Constipation. Difficulty passing stool may be due to painful blisters in the anal area. It can also be caused by not ingesting enough liquids or high-fiber foods, such as fruits and vegetables.
- Dental problems. Tooth decay and problems with tissues inside the mouth are common with some types of epidermolysis bullosa.
- Skin cancer. Teenagers and adults with certain types of epidermolysis bullosa are at increased risk of a type of skin cancer called squamous cell carcinoma.
- Death. Infants with severe junctional epidermolysis bullosa are at high risk of infections and loss of body fluids from widespread blistering. Blisters in the mouth and throat also make it harder to eat and breathe. Many of these infants don't survive.
Prevention
It's not possible to prevent epidermolysis bullosa. But these steps may help prevent blisters and infection.
- Handle your child gently. Your infant or child needs cuddling, but be very gentle. To pick up a child with epidermolysis bullosa, place the child on soft material and give support under the buttocks and behind the neck. Don't lift the child from under the arms.
- Take special care with the diaper area. If your child wears diapers, remove the elastic bands and avoid cleansing wipes. Line the diaper with a nonstick dressing or spread it with a thick layer of zinc oxide paste.
- Keep the home environment cool. Try to keep your home cool and the temperature steady.
- Keep the skin moist. Gently apply moisturizer as needed throughout the day.
- Dress your child in soft clothes. Use soft clothing that's simple to get on and off. It may help to remove labels and put on clothing seam-side out to reduce scratching. Try sewing foam pads into the lining of clothing by elbows, knees and other pressure points. Use soft special shoes, if possible.
- Prevent scratching. Trim your child's fingernails regularly.
- Encourage your child to be active. As your child grows, encourage activities that reduce the risk of skin injury. Swimming is a good option. For children with mild forms of epidermolysis bullosa, they can protect the skin by wearing long pants and sleeves for outdoor activities.
- Cover hard surfaces. Consider padding a car seat or bathing tub with sheepskin, foam or a thick towel. Soft cotton or silk can be used as a top layer over the padding.
Aug. 20, 2022