Overview
If you and your partner are struggling to have a baby, you're not alone. Millions of people around the world face the same challenge. Infertility is the medical term for when you can't get pregnant despite having frequent, unprotected sex for at least a year for most couples.
Infertility may happen because of a health issue with either you or your partner, or a mix of factors that prevent pregnancy. But many safe and effective treatments can boost your chances of getting pregnant.
Symptoms
The main symptom of infertility is not getting pregnant. There may be no other clear symptoms. Some women with infertility may have irregular menstrual periods or no periods. And some men may have some symptoms of hormonal problems, such as changes in hair growth or sexual function.
Many couples eventually will conceive — with or without treatment.
When to see a doctor
You likely don't need to see a member of your healthcare team about infertility unless you've been trying to get pregnant for at least one year. But women should talk with a healthcare professional sooner if they:
- Are age 35 or older and have tried to conceive for six months or longer.
- Are over age 40.
- Have no periods, or irregular or very painful periods.
- Have known fertility problems.
- Have endometriosis or a history of pelvic inflammatory disease.
- Have had more than one miscarriage.
- Have gotten cancer treatment such as chemotherapy or radiation.
Men should talk to a healthcare professional if they have:
- A low number of sperm or other problems with sperm.
- A history of testicular, prostate or sexual conditions.
- Had treatment for cancer such as chemotherapy.
- Had hernia surgery.
- Testicles that are smaller than the typical adult size, or swollen veins in the bag of skin that holds the testicles, called the scrotum.
- Had infertility with a partner in the past.
- Relatives with infertility problems.
Causes
Fertilization and implantation

Fertilization and implantation
During fertilization, the sperm and egg unite in one of the fallopian tubes to form a zygote. Then the zygote travels down the fallopian tube, where it becomes a morula. Once it reaches the uterus, the morula becomes a blastocyst. The blastocyst then burrows into the uterine wall — a process called implantation.
Male reproductive system

Male reproductive system
The male reproductive system makes, stores and moves sperm. The testicles produce sperm. Fluid from the seminal vesicles and prostate gland combines with sperm to make semen. The penis ejaculates semen during sexual intercourse.
Female reproductive system
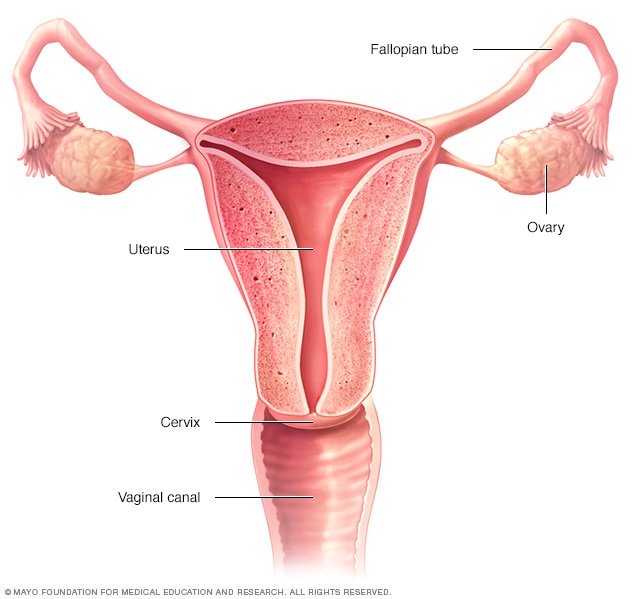
Female reproductive system
The ovaries, fallopian tubes, uterus, cervix and vagina (vaginal canal) make up the female reproductive system.
All of the steps during ovulation and fertilization need to happen correctly in order to get pregnant. Ovulation is the release of an egg from an ovary. Fertilization is when the egg and sperm unite to form an embryo, which becomes an unborn baby during pregnancy. Sometimes, the issues that cause infertility in couples are present at birth. Other times, they develop later in life.
Infertility causes can affect one or both partners. In some cases, no cause can be found.
Causes of male infertility
These can include:
- Conditions that can affect how much sperm is made or sperm quality. These medical conditions can include undescended testicles, genetic defects, hormone problems and health problems such as diabetes. Infections such as chlamydia, gonorrhea, mumps or HIV also can impact sperm. Enlarged veins in the scrotum, called a varicocele, can affect sperm's quality.
- Problems with sperm reaching the female reproductive tract. These issues can be due to sexual conditions such as premature ejaculation, certain genetic diseases such as cystic fibrosis, physical problems such as a blockage in the testicle, or damage or an injury to the reproductive organs.
- Certain factors in the environment. Exposure to pesticides, other chemicals or radiation can affect fertility. So can medicines that treat bacterial infections, high blood pressure and depression. And if the testicles often are exposed to heat, such as in saunas or hot tubs, that may affect their ability to make sperm.
- Damage related to cancer and its treatment. Cancer treatments such as chemotherapy and radiation can affect sperm production.
Causes of female infertility
These can include:
- Ovulation disorders. These conditions affect the release of eggs from the ovaries. They include hormonal problems such as polycystic ovary syndrome. High levels of a hormone needed to make breast milk, called prolactin, also may have an effect on ovulation. Either too much thyroid hormone, called hyperthyroidism, or too little, called hypothyroidism, can affect the menstrual cycle or cause infertility. Other underlying causes may include too much exercise, eating disorders or tumors.
- Conditions of the uterus. These include growths called uterine polyps, issues with the shape of the uterus or problems with its lower end, called the cervix. Tumors in the wall of the uterus, called uterine fibroids, also may cause infertility — but they aren't cancer. Fibroids can block the fallopian tubes, where an egg and sperm unite. They also can stop a fertilized egg from attaching to the uterus, which needs to happen for an unborn baby to develop.
- Fallopian tube damage or blockage. Often, these issues are caused by swelling of the fallopian tube, called salpingitis. The swelling can happen due to an infection of the female reproductive organs called pelvic inflammatory disease.
- Endometriosis. With this condition, tissue that's similar to the inner lining of the uterus grows outside of the uterus. It may affect the how well the ovaries, uterus and fallopian tubes work.
- Primary ovarian insufficiency. This happens when the ovaries stop working as they should, and menstrual periods end before age 40. The cause is often unknown. But some factors linked with primary ovarian insufficiency include immune system diseases, genetic conditions such as Turner syndrome, and radiation or chemotherapy treatment.
- Pelvic adhesions. These are bands of scar tissue that bind organs. They can form after a pelvic infection, appendicitis, endometriosis, or surgery of the abdomen or pelvis.
- Cancer and its treatment. Certain cancers — especially ones that affect the reproductive organs — often reduce female fertility. Both radiation and chemotherapy may affect fertility as well.
Risk factors
Many of the risk factors for both male and female infertility are the same. They include:
- Age. Women's fertility slowly declines with age, especially in the mid-30s. It drops quickly after age 37. Infertility in older women likely is due to the lower number and quality of eggs, or to health problems that affect fertility. Men over age 40 may be less fertile than younger men. The risk of birth defects and genetic problems also rises for children born to men over age 40.
- Tobacco use. Smoking tobacco by either partner may lower the chances of pregnancy. It also can make fertility treatments less effective. The risk of miscarriages may rise in women who smoke tobacco. When a pregnant person's partner smokes, that also raises the risk of miscarriage — even when the pregnant person is not a smoker. And smoking can raise the risk of erectile dysfunction and a low sperm count in men.
- Marijuana use. Marijuana may affect fertility, but more research is needed. Use during pregnancy has been linked with negative health effects on unborn babies. It also might raise the risk of miscarriage and stillbirth.
- Alcohol use. For women, there is no safe level of alcohol use when you're trying to get pregnant or during pregnancy. Alcohol may contribute to infertility. For men, heavy drinking can lower sperm count and affect how well sperm move.
- Being overweight. An inactive lifestyle and being overweight or obese can raise the risk of infertility. Obesity is linked with lower quality of semen, the fluid that contains sperm.
- Being underweight. People at risk of fertility problems include those with eating disorders, such as anorexia or bulimia. Those who follow a very low-calorie or restrictive diet also are at risk.
- Exercise issues. A lack of exercise plays a role in obesity, which raises the risk of infertility. Less often, ovulation problems may be linked with frequent, strenuous, intense exercise in women who are not overweight.
Prevention
Some types of infertility can't be prevented. But the following tips may boost your chances of pregnancy.
Couples
Have sex often soon after menstrual bleeding stops. One of the ovaries usually releases an egg in the middle of the cycle — halfway between menstrual periods — for most people with menstrual cycles about 28 days apart. It's ideal to have sex every day starting 5 to 7 days before the release of the egg. Continue until two days after ovulation.
Men
Most types of infertility aren't preventable in men, but these tips may help:
- Stay away from drugs and tobacco, and don't drink a lot of alcohol. Doing illegal drugs, smoking or drinking heavily can raise the risk of male infertility.
- Don't take frequent baths in hot water. The high temperatures can have a short-term effect on sperm production and movement.
- Stay away from pollutants and toxins. These include pesticides, lead, cadmium and mercury. Being exposed to them can affect the body's ability to make sperm.
- Limit medicines that may impact fertility if possible. Talk with your health care team about any medicines you take regularly. Don't stop any taking prescription drugs without medical advice.
- Work out. Regular exercise may improve sperm quality and boost the chances of a pregnancy.
Women
For women, the following tips may boost the chances of getting pregnant:
- Quit smoking. Tobacco has many bad effects on fertility. It's also terrible for your health and the health of an unborn baby. If you smoke and you want to try to become pregnant, quit tobacco now. You can ask your health care team for help.
- Stay away from alcohol and street drugs. These substances could make you less likely to conceive and have a healthy pregnancy. Don't drink alcohol or use recreational drugs, such as marijuana, if you're trying to get pregnant.
- Limit caffeine. Some women may need to cut back on caffeine when they try to get pregnant. Asks your health care team for advice. During pregnancy, many experts recommend you have no more than 200 milligrams of caffeine per day. That's about the amount in a 12-ounce cup of brewed coffee. Check food labels for amounts of caffeine too. The effects of caffeine aren't clear for an unborn baby. But the effects of higher amounts may include miscarriage or preterm birth.
- Exercise safely. Regular exercise is key for good health. But working out too intensely could cause your periods to happen less often or go away, and that could affect fertility.
- Get to a healthy weight. Being overweight or underweight can affect your hormones and cause infertility.
Sept. 13, 2023