Overview
Pulmonary embolism
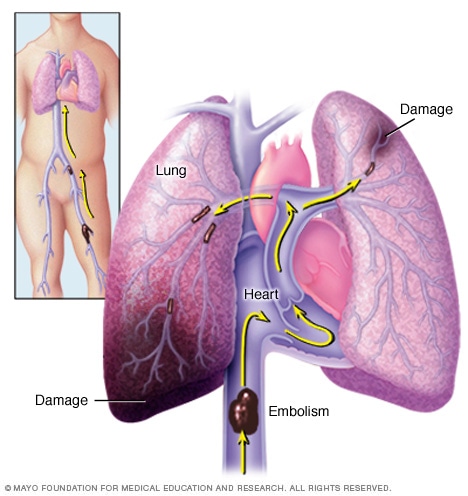
Pulmonary embolism
A pulmonary embolism (PE) occurs when a blood clot gets stuck in an artery in the lung, blocking blood flow to part of the lung. Blood clots most often start in the legs and travel up through the right side of the heart and into the lungs. This is called deep vein thrombosis (DVT).
A pulmonary embolism is a blood clot that blocks and stops blood flow to an artery in the lung. In most cases, the blood clot starts in a deep vein in the leg and travels to the lung. Rarely, the clot forms in a vein in another part of the body. When a blood clot forms in one or more of the deep veins in the body, it's called a deep vein thrombosis (DVT).
Because one or more clots block blood flow to the lungs, pulmonary embolism can be life-threatening. However, prompt treatment greatly reduces the risk of death. Taking measures to prevent blood clots in your legs will help protect you against pulmonary embolism.
Products & Services
Symptoms
Pulmonary embolism symptoms can vary greatly, depending on how much of your lung is involved, the size of the clots, and whether you have underlying lung or heart disease.
Common symptoms include:
- Shortness of breath. This symptom usually appears suddenly. Trouble catching your breath happens even when resting and gets worse with physical activity.
- Chest pain. You may feel like you're having a heart attack. The pain is often sharp and felt when you breathe in deeply. The pain can stop you from being able to take a deep breath. You also may feel it when you cough, bend or lean over.
- Fainting. You may pass out if your heart rate or blood pressure drops suddenly. This is called syncope.
Other symptoms that can occur with pulmonary embolism include:
- A cough that may include bloody or blood-streaked mucus
- Rapid or irregular heartbeat
- Lightheadedness or dizziness
- Excessive sweating
- Fever
- Leg pain or swelling, or both, usually in the back of the lower leg
- Clammy or discolored skin, called cyanosis
When to see a doctor
A pulmonary embolism can be life-threatening. Seek urgent medical attention if you experience unexplained shortness of breath, chest pain or fainting.
Causes
A pulmonary embolism occurs when a clump of material, most often a blood clot, gets stuck in an artery in the lungs, blocking the flow of blood. Blood clots most commonly come from the deep veins of your legs, a condition known as deep vein thrombosis.
In many cases, multiple clots are involved. The portions of lung served by each blocked artery can't get blood and may die. This is known as a pulmonary infarction. This makes it more difficult for your lungs to provide oxygen to the rest of your body.
Occasionally, blockages in the blood vessels are caused by substances other than blood clots, such as:
- Fat from the inside of a broken long bone
- Part of a tumor
- Air bubbles
Risk factors
Blood clot in leg vein
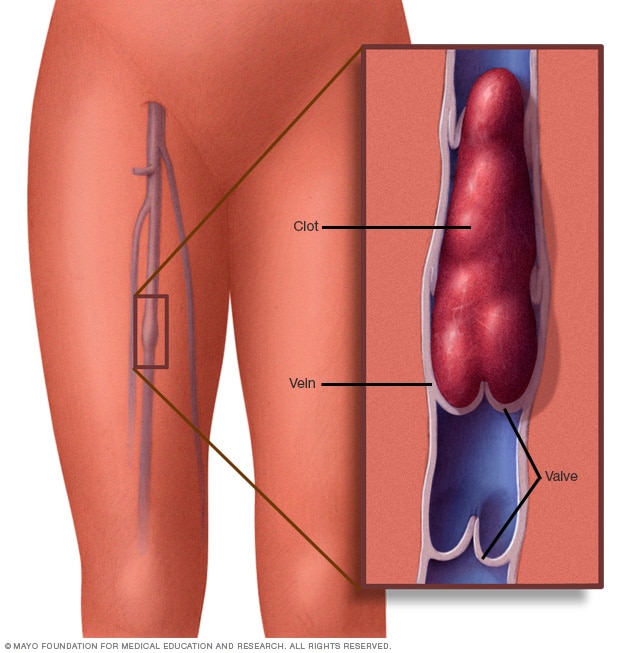
Blood clot in leg vein
A blood clot in a leg vein may cause swelling, pain, warmth and tenderness in the affected area.
Although anyone can develop blood clots that result in a pulmonary embolism, certain factors can increase your risk.
History of blood clots
You're at a higher risk if you or any of your blood relatives, such as a parent or sibling, have had venous blood clots or a pulmonary embolism in the past.
Medical conditions and treatments
Some medical conditions and treatments put you at risk, such as:
- Heart disease. Heart and blood vessel disease, specifically heart failure, makes clot formation more likely.
- Cancer. Certain cancers — especially brain, ovary, pancreas, colon, stomach, lung and kidney cancers, and cancers that have spread — can increase the risk of blood clots. Chemotherapy further increases the risk. You also have a higher risk of blood clots if you have a personal or family history of breast cancer and are taking tamoxifen or raloxifene (Evista).
- Surgery. Surgery is one of the leading causes of problem blood clots. For this reason, medicine to prevent clots may be given before and after major surgery, such as joint replacement.
- Disorders that affect clotting. Some inherited disorders affect blood, making it more likely to clot. Other medical disorders such as kidney disease also can increase the risk of blood clots.
- Coronavirus disease 2019 (COVID-19). People who have severe symptoms of COVID-19 have an increased risk of pulmonary embolism.
Extended periods of inactivity
Blood clots are more likely to form during longer than usual periods of inactivity, such as:
- Bed rest. Being confined to bed for an extended period after surgery, a heart attack, leg fracture, trauma or any serious illness puts you at risk of blood clots. When your legs lie flat for long periods of time, the flow of blood through your veins slows down and blood can pool in your legs. This sometimes can result in blood clots.
- Long trips. Sitting in a cramped position during lengthy plane or car trips slows blood flow in the legs, which increases the risk of blood clots.
Other risk factors
- Smoking. For reasons that aren't well understood, tobacco use increases the risk of blood clots in some people, especially those who have other risk factors.
- Being overweight. Excess weight increases the risk of blood clots — particularly in people with other risk factors.
- Supplemental estrogen. The estrogen in birth control pills and in hormone replacement therapy can increase clotting factors in the blood, especially in those who smoke or are overweight.
- Pregnancy. The weight of a baby pressing on veins in the pelvis can slow blood return from the legs. Clots are more likely to form when blood slows or pools.
Complications
A pulmonary embolism can be life-threatening. About one-third of people with an undiagnosed and untreated pulmonary embolism don't survive. When the condition is diagnosed and treated promptly, however, that number drops dramatically.
Pulmonary embolisms also can lead to pulmonary hypertension, a condition in which the blood pressure in the lungs and in the right side of the heart is too high. When you have blockages in the arteries inside your lungs, your heart must work harder to push blood through those vessels. This increases blood pressure and eventually weakens your heart.
In rare cases, small clots called emboli remain in the lungs and scarring develops in the pulmonary arteries over time. This restricts blood flow and results in chronic pulmonary hypertension.
Prevention
Preventing clots in the deep veins in your legs will help prevent pulmonary embolisms. For this reason, most hospitals are aggressive about taking measures to prevent blood clots, including:
- Blood thinners (anticoagulants). These medicines are often given to people at risk of clots before and after surgery. Also, they're often given to people admitted to the hospital with certain medical conditions, such as heart attack, stroke or complications of cancer.
- Compression stockings. Compression stockings steadily squeeze the legs, helping veins and leg muscles move blood more efficiently. They offer a safe, simple and inexpensive way to keep blood from pooling in the legs during and after surgery.
- Leg elevation. Elevating your legs when possible and during the night can be very effective. Raise the bottom of your bed 4 to 6 inches (10 to 15 cm) with blocks or books.
- Physical activity. Moving as soon as possible after surgery can help prevent pulmonary embolism and hasten recovery overall. This is one of the main reasons your nurse may push you to get up, even on your day of surgery, and walk despite pain at the site of your surgical incision.
- Pneumatic compression. This treatment uses thigh-high or calf-high cuffs that automatically inflate with air and deflate every few minutes. This massages and squeezes the veins in your legs and improves blood flow.
Prevention while traveling
The risk of blood clots developing while traveling is low but increases as long-haul travel increases. If you have risk factors for blood clots and you're concerned about travel, talk with your health care provider.
Your provider might suggest the following to help prevent blood clots during travel:
- Drink plenty of fluids. Water is the best liquid for preventing dehydration, which can contribute to the development of blood clots. Avoid alcohol, which contributes to fluid loss.
- Take a break from sitting. Move around the airplane cabin once an hour or so. If you're driving, stop every so often and walk around the car a couple of times. Do a few deep knee bends.
- Move in your seat. Bend and make circle movements with your ankles and raise your toes up and down every 15 to 30 minutes.
- Wear support stockings. Your provider may recommend these to help promote circulation and fluid movement in your legs. Compression stockings are available in a range of stylish colors and textures. There are even devices, called stocking butlers, to help you put on the stockings.
Dec. 01, 2022