Overview
Enlarged prostate

Enlarged prostate
Usually, the prostate gland is about the size and shape of a walnut or golf ball. When enlarged, the prostate may block the flow of urine from the bladder to the outside of the body.
Transurethral resection of the prostate (TURP) is a common surgery that's used to treat urinary problems that are caused by an enlarged prostate.
An instrument called a resectoscope is placed through the tip of the penis. It is then passed through the tube that carries urine from your bladder, called the urethra. The resectoscope helps a surgeon see and trim away extra prostate tissue that's blocking urine flow.
TURP tends to be considered an effective treatment choice for men who have moderate to serious urinary problems that haven't gotten better with medicine.
Other procedures that don't involve surgical cuts also are available to treat an enlarged prostate. Some of them work about as well as TURP. And in general, they cause fewer side effects and have a quicker recovery time.
Products & Services
Why it's done
TURP helps ease urinary symptoms caused by benign prostatic hyperplasia (BPH), including:
- Frequent, urgent need to urinate.
- Trouble starting urination.
- Slow or prolonged urination.
- More trips to the bathroom at night.
- Stopping and starting again while urinating.
- The feeling that you can't fully empty your bladder.
- Urinary tract infections.
TURP also might be done to treat or prevent complications due to blocked urine flow, such as:
- Repeated urinary tract infections.
- Kidney or bladder damage.
- Not being able to control urination or to urinate at all.
- Bladder stones.
- Blood in urine.
Risks
Risks of TURP can include:
- Short-term trouble urinating. This might last for a few days after the procedure. Until you can urinate on your own, you will need to have a thin, flexible tube called a catheter placed into your penis. It carries urine out of your bladder.
- Urinary tract infection. This type of infection can happen after any prostate procedure. It becomes more and more likely the longer you have a catheter in place. Some men who have TURP have repeated urinary tract infections.
- Dry orgasm. This is the release of semen during orgasm into the bladder rather than out of the penis. It's a common and long-term effect of any type of prostate surgery. Dry orgasm isn't harmful, and it doesn't tend to affect sexual pleasure. But it can make you less likely to get a female partner pregnant. Another name for it is retrograde ejaculation.
- Erectile dysfunction. This is trouble getting or keeping an erection. The risk is very small, but erectile dysfunction can happen after prostate treatments.
- Heavy bleeding. Very rarely, men lose enough blood during TURP that they need to receive donated blood through a vein. This is called a blood transfusion. Men with larger prostates seem to be at higher risk of heavy blood loss.
- Trouble holding urine. Rarely, loss of bladder control is a long-term side effect of TURP. It's also called incontinence.
- Low sodium in the blood, called hyponatremia. Rarely, the body absorbs too much of the fluid used to wash the surgery area during TURP. This can lead to having too much fluid and not enough sodium in the blood. When this happens, it's known as TURP syndrome or transurethral resection (TUR) syndrome. Without treatment, TURP syndrome can be life-threatening. A technique called bipolar TURP gets rid of the risk of this condition.
- Need for re-treatment. Some men need follow-up treatment after TURP. Their symptoms come back or don't get better over time. Sometimes, more treatment is needed because TURP causes the urethra or the bladder neck to narrow, also called a stricture.
How you prepare
Several days before surgery, your healthcare professional might recommend that you stop taking medicines that raise your risk of bleeding, including:
- Blood thinners such as warfarin (Jantoven) or clopidogrel (Plavix).
- Pain relievers sold over the counter, such as aspirin, ibuprofen (Advil, Motrin IB, others) or naproxen sodium (Aleve).
You might be prescribed medicine called an antibiotic to prevent a urinary tract infection.
Arrange to have a family member or friend drive you to and from the hospital. You won't be able to drive yourself home after the procedure that day or in general if you have a catheter in your bladder.
You might not be able to work or do strenuous activities for up to six weeks after surgery. Ask a member of your surgery team how much recovery time you might need.
What you can expect
The TURP procedure takes about 60 to 90 minutes to do. Before surgery you'll be given medicine that keeps you from feeling pain, called anesthesia. You might receive general anesthesia, which also puts you in a sleep-like state. Or you might get spinal anesthesia, which means you'll stay conscious. You also might be given a dose of antibiotics to prevent infection.
During the procedure
The resectoscope is placed into the tip of your penis. Then it's passed through your urethra and into your prostate area. Your surgeon won't need to make any cuts, also called incisions, on the outside of your body.
The resectoscope is used to trim tissue from the inside of the prostate gland. This is done one small piece at a time. As small pieces of tissue are cut from inside the prostate, the resectoscope also releases fluid. The fluid carries the pieces of tissue into the bladder. They're removed at the end of the operation.
After the procedure
Transurethral resection of the prostate (TURP)
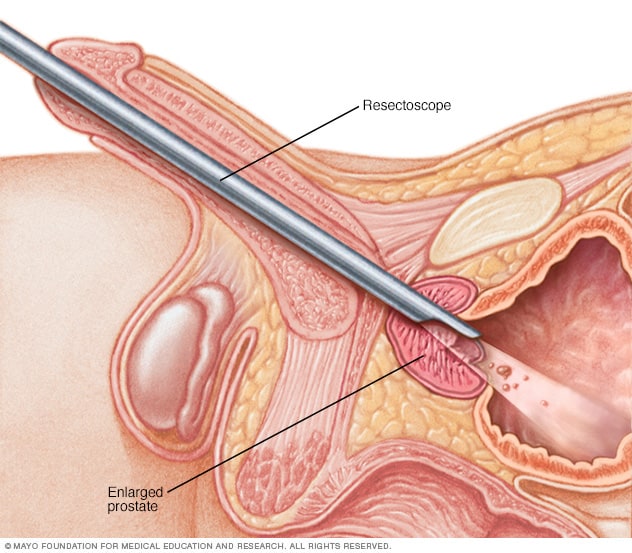
Transurethral resection of the prostate (TURP)
In transurethral resection of the prostate (TURP), a combined visual and surgical instrument (resectoscope) is inserted through the urethra where it's surrounded by prostate tissue. An electrical loop cuts away excess prostate tissue to improve urine flow.
You'll likely stay in the hospital for 1 to 2 days.
You'll have a urinary catheter in place because of swelling that blocks urine flow. Most often, the catheter is left in place for at least 24 to 48 hours, until swelling lessens and you're able to urinate on your own.
You might also notice:
- Blood in your urine. It's common to see blood right after surgery. Call your healthcare team if the blood in your urine is thick like ketchup, the bleeding seems to get worse or your urine flow is blocked. Blood clots can block urine flow.
- Other symptoms. Urination might be painful. Or you might feel an urgent or frequent need to urinate. Painful urination might take weeks to improve.
Your doctor is likely to recommend that you:
- Drink plenty of water to flush out the bladder.
- Eat high-fiber foods to prevent constipation and straining during a bowel movement. Your healthcare professional also might recommend a stool softener.
- Wait to resume taking any blood-thinning medicines until your healthcare team says it's OK.
- Stay away from strenuous activity, such as heavy lifting, for 4 to 6 weeks. Also during this time, do not do activities that put pressure on the area between the anus and the scrotum, such as riding a lawnmower.
- Hold off on sex for 4 to 6 weeks.
- Do not drive until your catheter is removed and you're no longer taking prescription pain medicines.
Call your healthcare team if you:
- Are not able to urinate.
- Notice bright red blood or clots in your urine.
- Notice that your urine isn't becoming clearer after drinking more fluid and resting for 24 hours.
Get medical care right away if you also have a fever or chills, or you feel lightheaded.
Results
TURP often relieves symptoms. The effects of treatment may last 15 years or longer. Follow-up treatment to ease symptoms is sometimes needed, particularly after several years have passed.
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.